Non sibi sed omnibus- Not for oneself, but for all
As you may already know, SoMe4Surgery celebrated its first birthday on the 28th of July 2019. More than a year has now passed since the birth of this dynamic surgical community and yet it continues to grow and flourish. As 2019 draws to a close, we take the opportunity to briefly reflect on what this year has brought to SoMe4Surgery and what we have to look forward to next year.

Fabulous factions and stellar societies
In keeping with the global trend of subspecialization in surgery, SoMe4Surgery has seen a rapid proliferation in the number of subgroups dedicated to various aspects of surgical practice. These range from broad specialties such as colorectal surgery, trauma and hepatopancreaticobiliary to finer and more specific fields like peritoneal surgery and bariatrics. Whatever your passion may be, you are bound to find the right surgical family to adopt you and your ideas. Just add the prefix SoMe4 and prepare to be amazed at what you will find in the treasure trove of Twitter societies at your disposal; these include exquisite rarities like mechanical ventilation, artificial intelligence in surgery, and genetic risk in cancer. And if, for some reason or another, you cannot find your El Dorado, you have the liberty to create one yourself complete with the blessings of the bigger SoMe4Surgery family.

The road to SMSS19
Perhaps the most memorable accomplishment in 2019 was the realization of the first SoMe4Surgery Summit in Madrid, now considered the surgical world’s Santiago de Compostela. Surgeons from all around the world flocked to Hospital Clinico San Carlos to participate by presenting and promoting their SoMe4Surgery experience. For those who could not physically make it, geography was no deterrent as they joined the virtual pilgrimage via live transmission online in what was an enjoyable and productive scientific journey. To celebrate the success of the day, participants later convened to dine and propose a toast in an evening that was christened SoMe4Fun.

You yourself can catch up on the details of that magical gathering and relive the excitement by looking up the hashtag #SMSS19 on Twitter. The event was a true testimony to the feasibility of virtualizing and subsequently de-virtualizing scientific and social networks.
Strength in solidarity
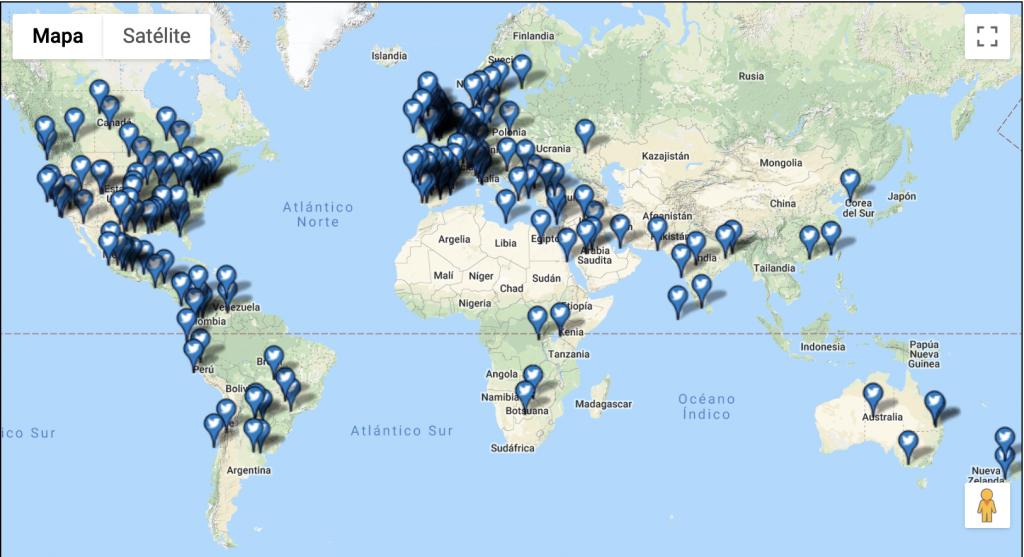
If you cannot go to SoMe4Surgery, then SoMe4Surgery will come to you. As surgeons recognize the importance of collaborating and sharing information and experiences in the 21st century, we have seen the hashtag #SoMe4Surgery being used alongside other hashtags in numerous conferences around the world; to name but a few: the American College of Surgeons Clinical Congress 2019, the European Society of Coloproctology Congress 2019 in Vienna, the Mexican General Surgery Association and the AIS Channel’s live colorectal surgery event. From workshops in cities as brilliant as Barcelona, as hot as Kuwait and as distant as Manila, you will find tweets that boast an intimate connection with SoMe4Surgery. Such collaborations have amplified the impact these conferences exert and have taken surgical knowledge where it has never gone before.
Power through publishing
While we will not attempt to list here the individual publications that have transpired through collaborative efforts within the SoMe4Surgery community, it suffices to mention that what once started as a tweet can now be found peer-reviewed and officially published in a number of reputable surgical journals. Real science mandates communication and cooperation and SoMe4Surgery provides a fertile ground to do just that. The power of the written word should not be underestimated and to generate meaningful publications has always been one of our goals.

Bilingual beyond borders
What Latin was to medicine in antiquity, English has become today. However, while English may be the lingua franca of our trade, this should not put the millions of non—English speaking professionals in the world at a disadvantage. This is why SoMe4Surgery now tweets in both English and Spanish culminating in an exponentially growing Hispanic surgical community that avidly shares its expertise. We hope to transcend language barriers through the help of multilingual colleagues as well as AI powered translators online. In defiance of philosopher Ludwig Wittgenstein’s infamous statement, at SoMe4Surgery, the limits of our language are not the limits of our world.
To infinity and beyond
“You have done so much with SoMe4Surgery already, what more is there to do?” you may ask.
While we cannot physically turn lead into gold, nor do we possess a crystal ball to foretell the exact future, we can make you one big promise though, and that is to continue to support surgeons, healthcare professionals and patients all around the world. Our alchemy lies in our ability to amalgamate the knowledge and expertise of everyone in SoMe4Surgery to create an ideal model of safe and scientifically sound surgical practice. Wherever you are, once you use the hashtag #SoMe4Surgery, we will find you and we will endorse you in whatever way we can.
We will continue to engage in active mentorship, to host educational activities on Twitter, to recruit colleagues and to share our experiences and discoveries through publications or otherwise, for the benefit of all-non sibi sed omnibus. Finally, we hope to see you all at the SoMe4Surgery Summit 2020, SMSS20.
*We would like to thank everyone who has been a member of this magnificent community, our pioneer surgeons who have continued to enrich our careers online as well as offline (including Professors Kenneth Mattox and Steven Wexner) and all the surgical journals and societies that have supported us unconditionally this year. We wish you and your families a safe and happy festive season, and a prosperous 2020, with SoMe4Surgery of course!



